The first and most important step in treating a person who is overdosing is to call 911, says a peer educator at the Melrose-based harm reduction and needle exchange program BOOM!Health, who spoke to the Herald on the condition of anonymity.
The hope is that emergency services will arrive soon after you’ve treated the person.
“But don’t tell them ‘My friend overdosed,’” the peer educator says. “They’ll take longer to come. Just say, ‘My friend stopped breathing.’”
Last year, more people died from drug overdoses in the Bronx, the fourth most populous of New York’s five boroughs, than in any other.
The community has taken an increased role in on-the-scene treatment of people who are overdosing. As of June of last year, 32 people in the Bronx had been treated in 2017 for overdoses by workers, volunteers, or members of Community Overdose Prevention (COP) programs like BOOM!, instead of by emergency service workers, according to the New York State Department of Health. That was already more than the borough’s 29 such cases in all of 2016. Last year’s number was second only to the 41 such cases in Manhattan, which is home to nearly 200,000 more people.
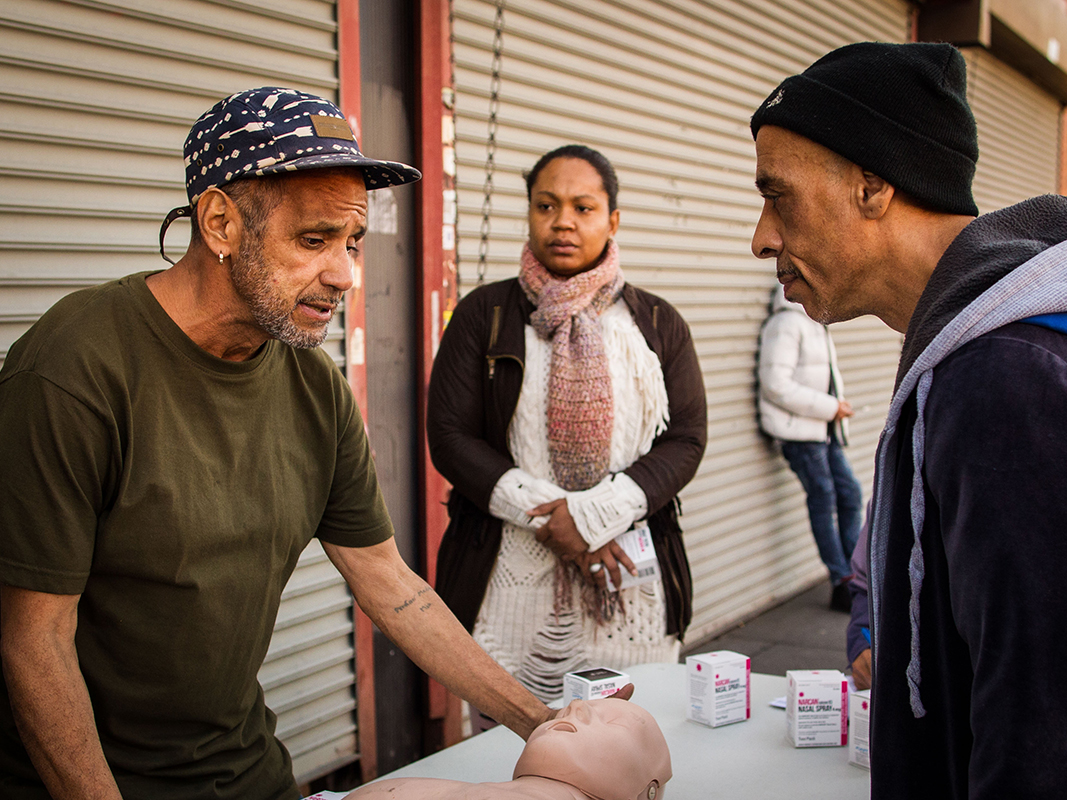
BOOM! offers a class that teaches community members how to administer a nasal spray version of naloxone, a pharmaceutical that reverses the effects of an opioid overdose. The drug’s brand name is Narcan; in November 2015 it became the first FDA-approved nasal spray remedy for opioid overdose developed for community use.
BOOM! peer educators teach the short class, which three reporters from the Herald have taken.
Two 4mg bottles of the drug come in a package; a single squeeze of the bottle releases a single dose of the drug.
The Narcan can take two to three minutes to take effect. Wait at least that long before administering another dose. Look for signs of consciousness – increased rate of breathing, movement, speech or sound.
“Keep your distance,” the peer educator warns. “They probably won’t be too happy with you,” as people coming out of an overdose are often disoriented.
The South Bronx has long suffered the community harm that accompanies opioid and, more specifically, heroin addiction: public overdoses, homeless encampments, unsafe play areas for children—parks are popular sites for drug users to get high. The battle reaches back to the ’60s, a peak in the area’s heroin crisis.
Now, after subsiding in the ’80s and ’90s, the the scourge of the drug has resumed with a new intensity, sparked by fentanyl, a synthetic opioid that is being used to pad batches of heroin and cocaine, as well as by prescription opioids. Experts at BOOM!Health say that fentanyl can be 50 to 100 times more powerful than heroin.
It’s the unpredictable presence of fentanyl that is causing users to overdose so violently.
BOOM! began offering fentanyl testing strips early last year, hoping that drug users will test their substances before injecting, says Alexis Brenes, a BOOM! official.
After being partially submerged – no farther than the blue line – in a mixture of water and the drug for about 15 seconds, the strips will reveal either one red stripe, indicating the presence of fentanyl, or two, suggesting the chemical’s absence. However, Brenes cautions, the strips are fallible.
“The strips are better than a guess,” he says. “If I look at it and try to tell you if it’s good or bad, that’s 50/50. [These strips are] better than that.”
Read our special series Opioid Addiction: Local Face on a National Crisis